The Real Reason Big Pharma Wants to Help Pay for Your Prescription – Bloomberg
Posted by My RAD Life in RA/RAD on August 3, 2016
RA, Fertility & Freezing Eggs
Posted by My RAD Life in Dealing, IVF / Egg Freezing, RA/RAD, Symptoms on July 24, 2016
Does rheumatoid arthritis effect fertility?
My fertility doctor thinks so, citing this study, but my rheumatologist disagrees. This lack on consensus means women aren’t counseled on this possibility by their rheumatologists and there is a general lack of information out there on the subject. But where does this uncertainty leave women like me, who are diagnosed with RA in the prime of our reproductive years.
In fact, women like me, who are diagnosed with RA before giving birth to their first child, have fewer children, possibly due to being on medications like methotrexate, which is linked to birth defects and therefore can’t be taken while trying to get/being pregnant or breastfeeding. It could also be because we’re choosing not to reproduce, fearing the burden of childbirth or raising a child with RA or passing our genes to our children.
It wasn’t until I was prompted by a gynecologist to test my ovarian reserve levels that I even gave this matter any thought. But now after being told my ovarian reserve is low, potentially due to RA, I do wish my rheumatologist would have told me to consider the possibility that my fertility might be effected by my RA earlier.
Had I considered this, I may have aligned my path to coincide with getting pregnant earlier or perhaps chosen to freeze my eggs earlier, a journey I’ve just set out on at age 33.
There are very few studies on the topic. This one, focusing on Systemic Lupus Erythematosus (SLE), found a higher correlation of SLE in infertile women than the general population, but the small sample size rendered the study inconclusive and its unknown if it would translate to women with other autoimmune diseases.
Others suggest that the higher incidence of inflammation which comes hand-in-hand with many autoimmune diseases could make it more difficult to carry a pregnancy to term. Autoimmune ID, a condition where your body’s immune system might attack an implanted embryo, resulting in a miscarriage, is more common in women with rheumatoid arthritis and other autoimmune disorders.
What’s more, it may take women with RA longer to get pregnant, perhaps due to trying to coordinate disease flares with needing to get off medications that would be harmful to the fetus.
Another thing to consider: autoimmune diseases may cause irregular ovulation, which can lead to more difficulty getting pregnant.
I don’t want to be too negative though, because many women with RA do successfully get pregnant and give birth, both naturally and through IVF. And one thing my rheumatologist and fertility doctor agree on is that, if anything, RA symptoms should lessen during IVF treatment as they do in pregnancy.
So what does this all mean? Does rheumatoid arthritis effect fertility? And what can we do about it?
Unfortunately, the answer is as unclear for me as when I started my research. I’ve taken all this inconclusive science, along with my own bloodwork showing low ovarian reserve, and my age (33), and have chosen to freeze my eggs with my partner’s support.
You’d think someone with RA would be used to their apartment being overrun by medications, but IVF takes it to a whole new level.
Here’s what my linen closet now looks like:

And here’s my fridge (my Enbrel now has company!):

And my kitchen counter:

I’m nervous about taking all the medications and what they might do to my RA symptoms, but I’m also feeling empowered about living in a time when I have the opportunity to freeze my eggs and get a bit of a fertility boost from science.
Worrying rise in accidental overdose of prescription drug methotrexate | smh.com.au
Posted by My RAD Life in RA/RAD on June 7, 2016
I’ve never understood why they make methotrexate and folic acid look nearly identical.
On vacation once, both bottles opened in my bag. I had to meticulously examine each yellow pill to sort them. Is this the little yellow pill (methotrexate) or the big yellow pill (folic acid)?
They should at least take the preventative measure of making these two very different drugs that are prescribed together different shapes and sizes.
RA & The Convoluted Path to Pregnancy
Posted by My RAD Life in Dealing, Drugs, IVF / Egg Freezing, RA/RAD, Relationships, Symptoms on May 21, 2016
I’m finally sitting down to write a review of Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May.

Now this little book is only 183 well-spaced pages and I started reading it way back in October. So what the heck took me so long?
To understand that, a bit of backstory…
As a child, I was never very into dolls. I liked climbing trees and playing ‘kick the can’. I obsessed over animals more than babies.
When I was 8, I got a new baby sister. When my parents first put her in my arms I thought she looked like a sick alien. Luckily she grew into the cutest toddler ever.
I think what I’m saying is, I was never one of those girls who solely dreamed of motherhood. In fact, growing up, I didn’t give it much thought. I just knew that someday I would become a mom. It seemed obvious, but it was not something I obsessed over.
When I was diagnosed with RA, single and 29 years old, my mind immediately went to my hypothetical future children. Was I already too late? Would this disease prevent me from having kids? Would it prevent me from meeting a significant other?
Luckily, the answer to those questions was ‘no’. Although, it did get a bit more complicated.
I started dating my current partner pretty much right after my diagnosis (well, this isn’t entirely true, because we had actually been exes, broken up for several years). It is in fact probably my RA that brought us back together.
The diagnosis softened me and made me more vulnerable, made me want to seek the support of those I truly loved, those who didn’t judge me. The people who truly rose to the top of that list were my mom and my ex-boyfriend. Go figure.
Four years later, we’re still together and wondering how four years have already passed. We’re getting more serious about “us” and those big life questions – What type of living situation do we want? Where do we see ourselves in 10 years? How do we feel about building a family?
My answer to that family question was largely one of emotion. I told my partner that I really wanted to build a family, become a mom. That this is something I always imagined for myself. In fact, given my childhood attitudes and how little I’d actually thought about this, I was surprised at the severity of my emotional attachment to becoming a mom.
His response was built more on logic and fear. One of six kids, he agreed that family was something he always assumed he would have someday, but he was concerned. What would pregnancy and parenthood look like for me, given my RA? What did it mean to get off the drugs? How would the hormones of pregnancy change the trajectory of my disease?
We spoke for a long time and I promised I would dig into it and find more information. I also promised that if my health was truly at risk, we’d look at another path, like adoption.
Problem is, there’s not a ton of info out there about this topic. Suzie Edward May’s book became the sole title on my list of books on the subject.
The book compiles many first person accounts of their path to parenthood with RA, including Suzie’s. It covers the challenge of getting off your RA meds to become pregnant. It covers the decision whether to stay off those drugs to breastfeed. It covers the possibility of a post-pregnancy flare.
It definitely made me feel less alone in my path. It made me feel scared and hopeful at the same time.
You won’t always succeed. There will be days and parts of days where you are fed up and sick of pain. Sick of thinking creatively about pain, sick of not being able to do what you want to do, and sick of always having to consider your health. But remember – you have dealt with worse before. Have a cry and then pick yourself up and keep moving forward.
– Excerpt from Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May
Suzie doesn’t sugarcoat the hard stuff. I appreciated that, but it drove home what my partner had been trying to tell me.
This isn’t going to be easy. There will be hard times. You have to really, really want this. And you have to be willing to accept Plan B if it’s not in the cards for us.
I’d finished the book, but I felt more lost than ever. I couldn’t yet compose my complicated emotions on the subject.
In fact, the questions I had that Suzie glosses over are perhaps the biggest ones of all. She assumes that you’re reading this because you need kids. You have that drive and you really want your own biological children. But how do you arrive at that first decision? How do you know that you’re ready to take on the challenge of pregnancy and parenthood and ADD to it with the complications of RA?
Then my annual exam in January brought with it some news: I have a low AMH. I know, WTH is that, right?
AMH, or anti-mullerian hormone, is thought to be a good reflection of your remaining egg supply. And mine was quite low for a 32-year-old woman (according to my gynecologist, there is disagreement on what these numbers really mean and their importance).
Your AMH levels decline as you age. According to my doctor, the level decreases by approximately 0.5 each year after the age of about 25. So my low number is on a steady march to menopause.
The other thing that decreases over time is the quality of your eggs. This is why many doctors recommend having kids before age 35.
This led me to a fertility clinic where they told me some good news: my AMH may be low, but my egg quality is excellent.
So what does this all mean? Well, it basically left my partner and I doing some figuring. We both believe siblings are important and would love to try for two kids. Given my RA, my pregnancies would have some extra time built in, meaning a timeline that looks like this:
- 3 months off methotrexate
- 1-12 months trying to get pregnant and being off methotrexate
- 9 months pregnant and off methotrexate and Enbrel
- 1-12 months potentially breastfeeding and off methotrexate and Enbrel (this is optional, as formula is available exactly for these situations!)
- get back on the drugs and recover
- rinse and repeat
At this point, I had turned 33 and my biological clock was like the relentless tick-tock in the crocodile in Peter Pan.
If I got off methotrexate now and started the path to pregnancy, it would be more than a year before I actually have a baby. Meaning baby number 2 is well over two years away. Given my dropping AMH, baby number 2 might not be an option at all. And this is assuming we are ready to start trying right now, which we’re just not.
So my partner and I are moving forward on freezing my eggs. This will give us an opportunity at baby number 2 (and number 1 if we run into difficulty), even if my AMH is non-existent. And future baby number 2 (and/or 1) will benefit from the “excellent” quality of my 33-year-old eggs.
This is not a decision we landed on lightly. There are no guarantees when it comes to egg freezing. It’s expensive and not even remotely covered by my insurance. I worried we were just creating another delay in our path to parenthood by not just going for it now. Along with those concerns, I still have to be off methotrexate for 2-3 months (at least 2 months before the freezing takes place), which was a pretty scary proposition.
I’m currently on week 5 off methotrexate and feeling empowered about my decision to freeze my eggs. The weeks have not been easy. My symptoms are definitely flaring. My days are stiff and even my knees, joints that have never been symptomatic for me before, are getting in on the action.
I was truly hoping that I would get off the drug and feel great, realize it really wasn’t helping and be able to live a life free of this not-so-fun medication. The silver lining is that I know the methotrexate was doing its job, suppressing my symptoms.
This convoluted path to parenthood, the big decisions, none of it is easy. But I’m ready to share my thoughts and my journey. I believe it’s all going to be worth it, and that is the whole point of Suzie’s book.
…make sure you have a full understanding of the impact the process could have on your life, be prepared and have action plans and support in place to deal with situations that may arise. Be open to things not going as you may desire. The more you are open to these types of things the less mental stress you will go through if things don’t go to plan.
– Mother of two with rheumatoid arthritis, Australia (excerpt from
Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May
When Hope is Gone
Posted by My RAD Life in RA/RAD on April 5, 2016
To RA patients like myself, drugs like Enbrel can feel like a miracle. Yes, we don’t want to rely on drugs, and, yes, there are side effects, and, sure, there are nasty warning labels. But the trade-off is life less limited by RA. Hope for a future that doesn’t include disability.
But that happily ever after is not the full story. Around 15-20% of Rheumatoid Arthritis patients have exhausted all the treatment options. The medications either result in too many side effects or become ineffective. For these patients, I imagine it feels like there’s not a lot of hope left.
A new drug just went through Phase 3 clinical trials that might offer these patients hope. Read more about it here.
Unmasked: Molecular Mechanism Of Rheumatoid Arthritis Revealed | Scope Blog
Posted by My RAD Life in RA/RAD on April 4, 2016
Design Thinking: Or Why Life with RA Forces You to be Creative
Posted by My RAD Life in Dealing, RA/RAD, Symptoms on February 26, 2016
Design Thinking:

Last night I went to a talk on Design Thinking. This is marketing/business jargon for approaching product design from a user’s point of view. The speaker encouraged everyone to go out and talk to their end-users so that they could design with empathy.
As an example, she talked about a new pill bottle that her company helped design. (Not sure what the product is, otherwise I’d post it.)
Her colleague went out and interviewed some older patients in their homes. Noticing an older woman’s severely arthritic hands, he asked her whether she had any trouble taking her medications at home. She replied that she had no problems at all.
He asked her to walk her through her medication routine, so she led him to her kitchen and showed him the electric meat slicer she used to open her pill bottles.
Yes, you read that right. She used this

to open these
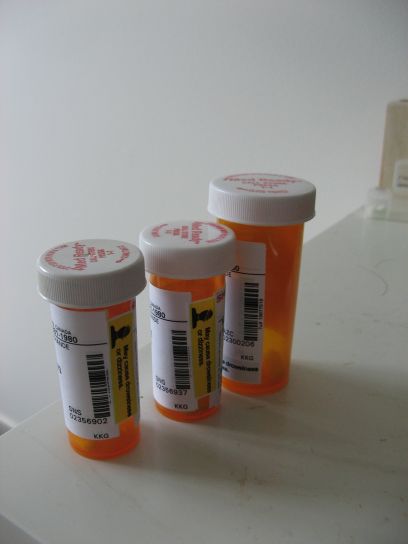
But the thing is, from her perspective – her “new normal” – she was doing just fine.
The product designer disagreed and apparently designed pill bottles that were easier to open.
This is a great little anecdote to encourage product designers to actually meet their intended product users, but that’s not really what I got out of it. I found this woman pretty damn inspiring. Here she is, with severe arthritis, and she’s making it work with the tools she has. She’s not whining. From her point of view, she’s just fine.
Design Thinking & RA:
This morning I was woken up by my right wrist, which was so stiff and painful I couldn’t move it. So I drag myself out of bed, take a really long, hot shower, and wait for my wrist to feel a bit better. No luck.
I dig out my wrist brace and attempt to brush my hair/teeth and apply make-up left-handed. Fun!
Then I go to work and try to operate my mouse with my left hand.
Now, I’m not as bad-ass as the woman in the story above. If anyone asked me if I was having trouble today, I’m pretty sure I would be a flood of complaints. But with diseases like RA, you’re forced to roll with the punches and get creative in how to compensate.
I’m happy to say that I went for a jog in the sun this afternoon and though still painful, my wrist is now doing a bit better (I’m typing this after all!).
Design Thinking as applied to life with RA:
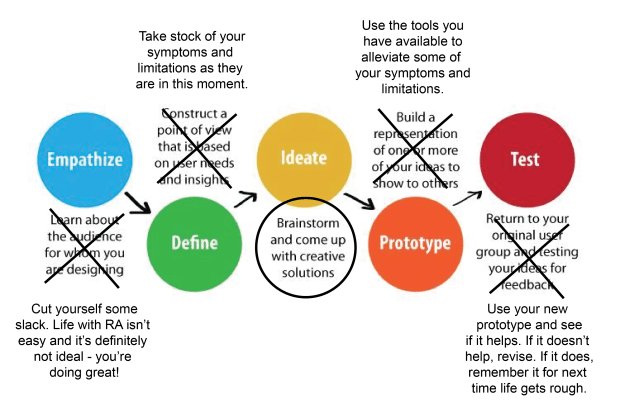
Have You Tried Fish Oil?
Posted by My RAD Life in Alternative Medicine, Dealing, Diet, Drugs, RA/RAD, Symptoms on February 23, 2016
I live in a city that embraces naturopaths, acupuncture and supplements. Anytime I tell anyone I have Rheumatoid Arthritis, they immediately follow with diet or supplement advice.
Fish oil cures that, right? MSM eliminates symptoms. Add turmeric!
This advice is not only coming from the uneducated. I’ve read books and studies recommending some supplements, including fish oil, from reputable sources.
When I was first diagnosed, I heeded this advice. It got to a point where I was taking a handful of pills morning and night.
Finally, my body had enough, which it communicated with a gag reflex I started getting just by seeing the vitamins in my hand. I’m currently listening to my body and taking just one supplement each day – alternating calcium/vitamin D with a hair, skin and nails formula (does wonders for my methotrexate-induced hair loss and weak nails!).
Last night, I finally got around to watching Frontline’s Supplements and Safety documentary.
It’s an important watch for anyone who adds supplements to their daily regimen.
I won’t pretend to be a doctor and offer medical advice. Some people get great results from supplements. Just please add them to your diet with caution and awareness that the industry is not regulated!
Choosing to Become a Parent with a Chronic Disease
Posted by My RAD Life in Dealing, RA/RAD, Relationships, Symptoms on October 16, 2015
I was diagnosed with Rheumatoid Arthritis or Rheumatoid Autoimmune Disease when I was 29. It’s an awkward age to be told you have a chronic disease.
There was so much I hadn’t yet accomplished. At the time, I was single, struggling to get my business off the ground, training for a marathon, and pushing thoughts of kids and marriage into the future. And then, a diagnosis of RA threw all that up in the air.
I feel like the pieces are still settling, four years later.
I got back together with a long-term boyfriend, largely because of my diagnosis. When I needed him, he was there without question. All the issues we’d had in the past paled to how much we obviously cared for each other, and that remains true today.
I pushed through a lot of ups and down and pain to cross the finish line of my first marathon. Today, I still run. Though training for a second marathon has faltered twice due to pain, I still have it in the back of my mind as a goal.
I tried to manage my business, while attempting to lower stress (doctors orders, and so much easier said than done in the world of start-ups!). The business is now doing better than ever, but stress management remains a constant struggle.
And then there’s kids…
I always figured I’d be a mother someday. I was never in a rush about it, but down the line, raising a family was always something I imagined for myself. After my diagnosis of RA, I suddenly found myself in a new reality.
When you have a name for the pain you’ve been experiencing, it becomes unavoidably real. There was no more blaming running or snowboard injuries. I couldn’t blindly keep pushing myself. I had pain walking and writing, bone erosions that no amount of medication could erase, extreme fatigue that was even causing me to fall asleep at work, a whacked-out GI tract that led to weight loss and avoiding eating all together, and depression because I had no idea why any of the above were happening to me. With a diagnosis came the answer of why, but it also brought the necessity to slow everything down and focus on getting better.
The new reality also meant being placed on strong drugs to control my symptoms, including a chemotherapy drug that is used to induce abortions in ectopic pregnancies. This particular drug requires women to be off of it for an extended period of time before even attempting to get pregnant.
Suddenly, I was far less sure I would ever be a parent. Four years of focusing on my health, coming to terms with living with chronic disease, and finding a new normal has given me the space to seriously revisit the question of parenthood.
Huge questions still exist for me. These are questions that only those of us living with chronic illness and our partners can understand.
Will I be healthy enough to go through pregnancy? If I ween off my RA drugs, will I return to the level of pain I was at pre-diagnosis? Will I be able to stay off the drugs long enough to breastfeed? If I can successfully have one child, will I be able to have another? Will pregnancy make my symptoms worse or better? Will post-pregnancy change my disease trajectory? Will the drugs I’m on be as effective post pregnancy? Will my RA slow me down as a parent? Will I pass the genetic disposition for autoimmune diseases on to my kids?
To help me navigate the complexities of this big decision, I’m reading Arthritis, Pregnancy and the Path to Parenthood by Suzie Edward May.
I’ve only just started the book, but I already identify with Suzie so well. She was diagnosed at 27 before having kids. The book offers a lot of hope, but also non-sugar-coated truth. I’ll give a more complete review when I finish it.
In the meantime, can anyone weigh in on what factors you looked at when deciding to become a parent while living with a chronic disease?
But You’re Better, Right?
Posted by My RAD Life in Dealing, RA/RAD on September 9, 2015
First off, my apologies for being off the radar for, well, months.
My work has been busy and I’ve been trying to finish up my second novel. (If anyone has any interest in checking out my first book, you can find it here.)
It’s left me with little motivation to write this blog after busy days that include a lot of time in front of the computer. In fact, I’ve spent many nights these past few months just being exhausted and having a great relationship with Netflix.
On to the good stuff.
I was recently at a dinner and found out through that a person close to me might have Lyme Disease. I was listening to her symptoms – sore joints, fatigue, depression – and told her I understand how a lot of these symptoms feel and that she should call me if I want to talk.
To which she responded, “But you’re better, right?”
She’s not the first person I’ve heard this from. I’ve heard it from friends and family, those who should really understand chronic disease better. And I get it. They see me and I look healthy — I go to work, get exercise, write, travel. I don’t complain like I used to before I had a diagnosis.
I’m better, right?
Well, not exactly. “Better” suggests “cured” and I think that’s how most people mean it. But in the world of chronic disease and Rheumatoid Arthritis, cured is not really part of our reality (Yet! So much exciting medical research is happening right now!).
So how can you balance educating people, but not causing those close to you worry -OR- come off as complaining?
Honestly, I’m not sure.
I responded by saying that my drug therapy allows me to manage my disease and I feel much, much better than I did before treatment. This is the truth. I balance pain, fatigue, new limits, and, yes, even depression from time to time. I tweak my drug regimen constantly to take the least amount of drugs possible while managing my pain. I take two heavy-duty drugs weekly just to keep a semi-normal life and I get blood panels regularly to make sure my liver’s keeping up.
I don’t feel cured, but I do feel better.
So, what about you? How do you handle the “Aren’t you better yet?” line?

Hopefully we all respond better than this to the “feeling better” question! I just thought this one was funny!


