Archive for category Dealing
Heroes
Posted by My RAD Life in Dealing, Symptoms on March 2, 2019
Selma Blair is such an inspiration. Not only was she stunning at the Oscars, her raw, honest interview on Good Morning America was so courageous.
Traveling with [RA] Drugs
Posted by My RAD Life in Dealing, Drugs, RA/RAD on September 27, 2018
Lordy, it’s been a hot minute! I can’t believe how much time has passed since my last post, which I can only attribute to my switch from Enbrel to Cimzia, which has me feeling perfectly healthy. And, feeling healthy means writing an RA blog is not top of mind.
This summer I found myself traveling quite a lot. As my readers will know, I’ve done a lot of traveling with Enbrel, which has been approved to safely remain out of the fridge for two weeks (a traveler’s dream!).
Cimzia is another story……
Part I – A Trail of Water

So, I packed up my three month’s worth of drugs with ice packs and spare Ziplocs for the ice I knew I’d need on my journey to Berlin – a domestic flight, a three-hour layover, an international flight, a twelve-hour layover, a taxi ride —> finally, fridge in Berlin, Germany.
Most airlines will not help you out by putting freezer packs in a freezer or drugs in a refrigerator during your flight. American Airlines was no different, but they did give me ice in a bucket, which helped a bit. But byy the time I got to Zurich, just halfway through my journey, my ice packs were dripping and I was worried about my drugs warming up.
I got off the plane in Zurich and immediately went on a mission for a waterproof cooler and ice. Apparently these things are hard to find…. I ultimately found ice at a restaurant, but not a cooler – even after being in grocery stores and pharmacies.
So me and my cloth cooler and dripping bags of ice went on a tour around the city, leaking water every step we took. I stopped at many cafes, got dirty looks from many waitresses as I asked for ice, and alternated between cursing my drugs and being grateful that I had them so I could travel at all.
I felt a huge relief getting them in the refrigerator in Berlin – their home for a month and a half.

Part II – This Bar Has Ice…. and Alcohol

I met my parents in the Netherlands and the hotel they booked didn’t have a refrigerator. For a ormal traveler, this wouldn’t matter in the least. For someone traveling with drugs that have to be refrigerated, it’s a total pain.
We got in late so the lobby was closed. I talked my mom into walking to a bar to try to convince the bartender to give me a few bags of ice (and, you know, maybe grab a drink or two).
We lucked out and got a late night glass of wine and enough ice to sustain me until the lobby and kitchen opened up and I could stash my RA drugs in the kitchen fridge.
Part III – So Much For the Good Seats

I flew from Germany to France to meet my friend in Bordeaux. The journey included a flight and long train ride, but at this point I’d gotten used to it and had plenty of ice packs to get me through the journey. At the hotel, I realized we didn’t have a refrigerator in our room (again!), so I asked the hotel to store my drugs, which they graciously did.
When it was time to depart to the coastal town of Biarritz, we were running late. We checked out in a rush, Ubered to the train station and sat down with relief that we made it. It was about the time that we were celebrating the proximity of our seats to the bar car that I realized I’d left my Cimzia in the hotel fridge.
“I left my drugs, I’ll meet you in Biarritz!” is all I had time to say as I grabbed my backpack and bolted off the train just in time to see it leave.
I took a cab back to the hotel, grabbed my drugs, cabbed back to the train station, realized my tickets were non-refundable and the next train wasn’t for awhile, booked a bus ticket, waited for a bus that was two hours late, and finally made it…..
Part IV – No Pain, No Gain
Yes, traveling with RA drugs is a pain. I wish I didn’t have to do it. But I am so grateful I get to travel. I am so grateful my joints are strong enough to grab a bag and run off a train. I am so grateful I am health enough to wander around Zurich for twelve hours. Drippy ice packs or not, I can only channel gratitude. I hope that RA drugs don’t stop you from going to the places you want to go!
My Month on the AIP Diet
Posted by My RAD Life in Alternative Medicine, Autoimmune Protocol Diet, Dairy/Casein Free, Dealing, Diet, Gluten Free, RA/RAD, Recipes, Symptoms on March 26, 2018
If you live with a chronic disease, you’ve been told some variation of “you can cure your disease if you eat this or don’t eat this”. I’ve been told to eat ginger, turmeric, be vegan, go paleo, cut dairy, cut nightshades.
The list goes on, and I’m generally skeptical of these suggestions. But there’s nothing like mounting symptoms to get you to try anything.
So last fall, I decided to embrace the Autoimmune Protocol completely for 30 days and slowly add in foods. To help, I bought
- The Autoimmune Wellness Handbook: A DIY Guide to Living Well with Chronic Illness
- The Autoimmune Paleo Cookbook: An Allergen-Free Approach to Managing Chronic Illness
The diet is strict – essentially having you cut anything that could trigger a reaction, reset your gut, and add foods back one by one.
Here’s the guide I followed, created by Mickey Trescott:


After a month of following the diet, and a few months adding foods back in, here’s what I learned:
- Life is just not the same without coffee and wine. 😉 Seriously, I don’t care if my symptoms flare a bit, these “food groups” have been added back and are staying.
- The diet makes eating out nearly impossible. For me, this was difficult as I eat out a lot. Being forced to cook so much was a learning curve, but I’m now a much better cook!
- I now know how to cook all sorts of meats. Before this diet, my kitchen was essentially vegetarian because I didn’t like cooking meat. Now I cook it weekly.
- Nightshade vegetables DO cause achy joints for me the next day, particularly tomatoes and peppers.
- My gut feels better with WAY fewer grains in my diet. Though I’m currently not gluten free, I generally now stick to rice and corn if I’m eating grains.
- I have continued to eat more vegetables, meat, fermented foods and kombucha and feeling better for it. Most mornings, I still make myself a green smoothie to start the day.
I’m not about to tell you this diet will cure you. I’m feeling better, but I think that’s largely due to a change in medication (switching from Enbrel to Cimzia). Adding the “light” version of this diet I’ve landed on to my lifestyle keeps me healthy and makes me feel good. I recommend testing it for yourself and would love to hear if you have experience with this diet in the comments!
Back Here Again
Posted by My RAD Life in Alternative Medicine, Dairy/Casein Free, Dealing, Diet, Doctors, Drugs, Gluten Free, RA/RAD, Symptoms on May 31, 2017
“I just don’t know how much pain I’m expected to endure,” I confided to my friend.
And so, I had to admit to myself that I’ve been living with more pain, more morning stiffness, more burning sensations in my joints waking me up at night than I was willing to tolerate.
Because the pain is scary. It makes me think of my X-rays when I first got diagnosed, showing the pain that I had ignored had turned into bone erosions – permanent damage.
And because the pain is exhausting. Emotionally and physically exhausting. Invading my thoughts throughout the day. Throbbing right wrist, stiff left pinky, swollen left ankle, burning right elbow — Oh, was I supposed to be paying attention in this meeting? Invading my sleep at night. Invading my optimism that I had this disease under control.
And then I had to admit it to my rheumatologist. And then I heard him asking if I wanted to get on Prednisone. No. Methotrexate? I’d rather not….. I like a drink. I like to know if I get pregnant I won’t have to abort the child. I like not feeling nauseous one day a week and shedding copious amounts of hair. What else is there?
So now, Plaquenil. A malaria medication, which is a DMARD used to treat lupus and rheumatoid disease (though the printed information the pharmacist gave me states “they don’t know why it works to treat these diseases” — encouraging, right?).
Following the appointment came a struggle. Reading the side effects, wondering if more drugs were the right course, determining to also try lifestyle and diet changes.
Wondering if this was somehow because of something I could have prevented. Something I did. Eating the wrong thing? Stressing about my breakup and work too much? What if I could meditate and eat more kale? And cut out nightshade vegetables and gluten and dairy and sugar and caffeine and never drink again and basically become a monk? Would this disease leave me alone then?
And then depression. And acceptance. And sadness.
Because I’m back here again. Wondering if this treatment will work. Remembering that this disease is labeled chronic and I’m probably stuck with it for the rest of my life. Trying to remember how to feel optimistic and hopeful.
And two pills a day. And one shot a week. And less gluten, dairy, sugar, nightshade veggies, caffeine and alcohol. And more acupuncture.
And maybe starting to feel better. Maybe remembering how to have hope.
Love to all of you dealing with the taxing ups and downs of autoimmune diseases. I would not wish this on anyone, but it does force you to slow down, to be aware of your body, to appreciate the moments that are pain free and the moments where you surprise yourself with what you can do and what you can bear.
If anyone has experience with Plaquenil – good or bad, I’d love to hear it!
Embrace Yourself
Posted by My RAD Life in Dealing, RA/RAD, Uncategorized on November 30, 2016
Here’s a challenge: love your body.
I mean it. Dance in front of a mirror and tell yourself your beautiful.
Love your tall, your short, your skinny, your fat. Love your freckles, your dimples, your birth marks. Love your hips, your boobs, your butt.
Love your joints that don’t quite straighten. Love your rheumatoid nodules. Love your body’s quirks and imperfections.
I mean, why not?
Next time you catch yourself “if only-ing” about your body…. If only my eyes were blue. If only I lost 10 pounds. If only my face was perfectly symmetrical. And I was taller, thinner. And I could run without sweating. And eat without gaining weight. And stand on the beach as though salt water were a hair product.
If only….
Stop. It.
Breathe. Love. Embrace.
Eggs Over Easy
Posted by My RAD Life in Dealing, Drugs, IVF / Egg Freezing, RA/RAD, Symptoms on October 16, 2016

So, this is how it was supposed to go! Two painless weeks of hormones and 9 mature eggs now in the freezer.
After my canceled round a couple of months ago, I was feeling pretty discouraged. I took a month “off” to prep my body for a second round.
Of course, “off” in the world of fertility meant a month of testosterone gel, progesterone, estrogen, and blood thinners. So, the month off was taxing, but it let my brain take a break and forget about eggs.
Then, day one of my cycle came. The ultrasound brought news of another cyst. Last round, the cyst had been a showstopper and I chose to spend money to have it drained so I could continue with the hormones.
This time, the cyst was small enough that they gave me a choice: wait another month for it to go away, have it drained (for yet another $600), or continue with the hormones and risk the cyst growing as well.
My nurse told me to listen to my gut, and my gut was telling me that it had been a waste of money draining it last time and obviously my body is prone to cysts, so waiting it out didn’t seem rational. I opted to begin the hormones: Menopur, Omnitrope, Gonal-F and Clomid, this time at higher doses than the last round.
And this time around, in spite of the extra shots each day, I found it relatively easy. Giving myself shots wasn’t as emotionally taxing as last round and my body wasn’t bruising anymore (in spite of still being on blood thinners).
I eagerly awaited for day 6 when I could find out how my eggs were growing and whether the cyst was messing everything up. Last time the news on day 6 was that I only had four eggs growing, but two were so far behind, only two would be mature by my retrieval date. This time, I had 11 good-looking possibilities and my cyst was growing slowly enough not to be a concern.
After that, it was continued hormones, daily morning ultrasounds and bloodwork, and daily afternoon calls from the nurse. To my surprise, everything was growing right on schedule. My body was responding well and things were looking good.
Finally, I got the news that it was time to take my trigger shot. The shot had to be taken at exactly 8:30pm so that surgery could take place exactly 36 hours later. It was my fist time giving myself an intramuscular shot (versus subcutaneous) and I was super nervous. To my surprise, it was relatively painless (though I was pretty sore afterward).
My partner drove me to surgery 36 hours later and that went smoothly. No pain during or after and I didn’t even get sick from the anesthesia! I am very happy that we got 9 mature eggs (so much better than the 2 from last round!).
Seriously, after all the complications my body has thrown me, I was shocked that things just went well.
One major bonus of this whole process: I’m still off of methotrexate and my RA symptoms are under control. I still take Enbrel (and I will never complain about one shot per week again!), but my rheumatologist and I are going to try to keep me off methotrexate. I’m so excited to be down to one RA drug!!
RA, Fertility & Freezing Eggs
Posted by My RAD Life in Dealing, IVF / Egg Freezing, RA/RAD, Symptoms on July 24, 2016
Does rheumatoid arthritis effect fertility?
My fertility doctor thinks so, citing this study, but my rheumatologist disagrees. This lack on consensus means women aren’t counseled on this possibility by their rheumatologists and there is a general lack of information out there on the subject. But where does this uncertainty leave women like me, who are diagnosed with RA in the prime of our reproductive years.
In fact, women like me, who are diagnosed with RA before giving birth to their first child, have fewer children, possibly due to being on medications like methotrexate, which is linked to birth defects and therefore can’t be taken while trying to get/being pregnant or breastfeeding. It could also be because we’re choosing not to reproduce, fearing the burden of childbirth or raising a child with RA or passing our genes to our children.
It wasn’t until I was prompted by a gynecologist to test my ovarian reserve levels that I even gave this matter any thought. But now after being told my ovarian reserve is low, potentially due to RA, I do wish my rheumatologist would have told me to consider the possibility that my fertility might be effected by my RA earlier.
Had I considered this, I may have aligned my path to coincide with getting pregnant earlier or perhaps chosen to freeze my eggs earlier, a journey I’ve just set out on at age 33.
There are very few studies on the topic. This one, focusing on Systemic Lupus Erythematosus (SLE), found a higher correlation of SLE in infertile women than the general population, but the small sample size rendered the study inconclusive and its unknown if it would translate to women with other autoimmune diseases.
Others suggest that the higher incidence of inflammation which comes hand-in-hand with many autoimmune diseases could make it more difficult to carry a pregnancy to term. Autoimmune ID, a condition where your body’s immune system might attack an implanted embryo, resulting in a miscarriage, is more common in women with rheumatoid arthritis and other autoimmune disorders.
What’s more, it may take women with RA longer to get pregnant, perhaps due to trying to coordinate disease flares with needing to get off medications that would be harmful to the fetus.
Another thing to consider: autoimmune diseases may cause irregular ovulation, which can lead to more difficulty getting pregnant.
I don’t want to be too negative though, because many women with RA do successfully get pregnant and give birth, both naturally and through IVF. And one thing my rheumatologist and fertility doctor agree on is that, if anything, RA symptoms should lessen during IVF treatment as they do in pregnancy.
So what does this all mean? Does rheumatoid arthritis effect fertility? And what can we do about it?
Unfortunately, the answer is as unclear for me as when I started my research. I’ve taken all this inconclusive science, along with my own bloodwork showing low ovarian reserve, and my age (33), and have chosen to freeze my eggs with my partner’s support.
You’d think someone with RA would be used to their apartment being overrun by medications, but IVF takes it to a whole new level.
Here’s what my linen closet now looks like:

And here’s my fridge (my Enbrel now has company!):

And my kitchen counter:

I’m nervous about taking all the medications and what they might do to my RA symptoms, but I’m also feeling empowered about living in a time when I have the opportunity to freeze my eggs and get a bit of a fertility boost from science.
RA & The Convoluted Path to Pregnancy
Posted by My RAD Life in Dealing, Drugs, IVF / Egg Freezing, RA/RAD, Relationships, Symptoms on May 21, 2016
I’m finally sitting down to write a review of Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May.

Now this little book is only 183 well-spaced pages and I started reading it way back in October. So what the heck took me so long?
To understand that, a bit of backstory…
As a child, I was never very into dolls. I liked climbing trees and playing ‘kick the can’. I obsessed over animals more than babies.
When I was 8, I got a new baby sister. When my parents first put her in my arms I thought she looked like a sick alien. Luckily she grew into the cutest toddler ever.
I think what I’m saying is, I was never one of those girls who solely dreamed of motherhood. In fact, growing up, I didn’t give it much thought. I just knew that someday I would become a mom. It seemed obvious, but it was not something I obsessed over.
When I was diagnosed with RA, single and 29 years old, my mind immediately went to my hypothetical future children. Was I already too late? Would this disease prevent me from having kids? Would it prevent me from meeting a significant other?
Luckily, the answer to those questions was ‘no’. Although, it did get a bit more complicated.
I started dating my current partner pretty much right after my diagnosis (well, this isn’t entirely true, because we had actually been exes, broken up for several years). It is in fact probably my RA that brought us back together.
The diagnosis softened me and made me more vulnerable, made me want to seek the support of those I truly loved, those who didn’t judge me. The people who truly rose to the top of that list were my mom and my ex-boyfriend. Go figure.
Four years later, we’re still together and wondering how four years have already passed. We’re getting more serious about “us” and those big life questions – What type of living situation do we want? Where do we see ourselves in 10 years? How do we feel about building a family?
My answer to that family question was largely one of emotion. I told my partner that I really wanted to build a family, become a mom. That this is something I always imagined for myself. In fact, given my childhood attitudes and how little I’d actually thought about this, I was surprised at the severity of my emotional attachment to becoming a mom.
His response was built more on logic and fear. One of six kids, he agreed that family was something he always assumed he would have someday, but he was concerned. What would pregnancy and parenthood look like for me, given my RA? What did it mean to get off the drugs? How would the hormones of pregnancy change the trajectory of my disease?
We spoke for a long time and I promised I would dig into it and find more information. I also promised that if my health was truly at risk, we’d look at another path, like adoption.
Problem is, there’s not a ton of info out there about this topic. Suzie Edward May’s book became the sole title on my list of books on the subject.
The book compiles many first person accounts of their path to parenthood with RA, including Suzie’s. It covers the challenge of getting off your RA meds to become pregnant. It covers the decision whether to stay off those drugs to breastfeed. It covers the possibility of a post-pregnancy flare.
It definitely made me feel less alone in my path. It made me feel scared and hopeful at the same time.
You won’t always succeed. There will be days and parts of days where you are fed up and sick of pain. Sick of thinking creatively about pain, sick of not being able to do what you want to do, and sick of always having to consider your health. But remember – you have dealt with worse before. Have a cry and then pick yourself up and keep moving forward.
– Excerpt from Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May
Suzie doesn’t sugarcoat the hard stuff. I appreciated that, but it drove home what my partner had been trying to tell me.
This isn’t going to be easy. There will be hard times. You have to really, really want this. And you have to be willing to accept Plan B if it’s not in the cards for us.
I’d finished the book, but I felt more lost than ever. I couldn’t yet compose my complicated emotions on the subject.
In fact, the questions I had that Suzie glosses over are perhaps the biggest ones of all. She assumes that you’re reading this because you need kids. You have that drive and you really want your own biological children. But how do you arrive at that first decision? How do you know that you’re ready to take on the challenge of pregnancy and parenthood and ADD to it with the complications of RA?
Then my annual exam in January brought with it some news: I have a low AMH. I know, WTH is that, right?
AMH, or anti-mullerian hormone, is thought to be a good reflection of your remaining egg supply. And mine was quite low for a 32-year-old woman (according to my gynecologist, there is disagreement on what these numbers really mean and their importance).
Your AMH levels decline as you age. According to my doctor, the level decreases by approximately 0.5 each year after the age of about 25. So my low number is on a steady march to menopause.
The other thing that decreases over time is the quality of your eggs. This is why many doctors recommend having kids before age 35.
This led me to a fertility clinic where they told me some good news: my AMH may be low, but my egg quality is excellent.
So what does this all mean? Well, it basically left my partner and I doing some figuring. We both believe siblings are important and would love to try for two kids. Given my RA, my pregnancies would have some extra time built in, meaning a timeline that looks like this:
- 3 months off methotrexate
- 1-12 months trying to get pregnant and being off methotrexate
- 9 months pregnant and off methotrexate and Enbrel
- 1-12 months potentially breastfeeding and off methotrexate and Enbrel (this is optional, as formula is available exactly for these situations!)
- get back on the drugs and recover
- rinse and repeat
At this point, I had turned 33 and my biological clock was like the relentless tick-tock in the crocodile in Peter Pan.
If I got off methotrexate now and started the path to pregnancy, it would be more than a year before I actually have a baby. Meaning baby number 2 is well over two years away. Given my dropping AMH, baby number 2 might not be an option at all. And this is assuming we are ready to start trying right now, which we’re just not.
So my partner and I are moving forward on freezing my eggs. This will give us an opportunity at baby number 2 (and number 1 if we run into difficulty), even if my AMH is non-existent. And future baby number 2 (and/or 1) will benefit from the “excellent” quality of my 33-year-old eggs.
This is not a decision we landed on lightly. There are no guarantees when it comes to egg freezing. It’s expensive and not even remotely covered by my insurance. I worried we were just creating another delay in our path to parenthood by not just going for it now. Along with those concerns, I still have to be off methotrexate for 2-3 months (at least 2 months before the freezing takes place), which was a pretty scary proposition.
I’m currently on week 5 off methotrexate and feeling empowered about my decision to freeze my eggs. The weeks have not been easy. My symptoms are definitely flaring. My days are stiff and even my knees, joints that have never been symptomatic for me before, are getting in on the action.
I was truly hoping that I would get off the drug and feel great, realize it really wasn’t helping and be able to live a life free of this not-so-fun medication. The silver lining is that I know the methotrexate was doing its job, suppressing my symptoms.
This convoluted path to parenthood, the big decisions, none of it is easy. But I’m ready to share my thoughts and my journey. I believe it’s all going to be worth it, and that is the whole point of Suzie’s book.
…make sure you have a full understanding of the impact the process could have on your life, be prepared and have action plans and support in place to deal with situations that may arise. Be open to things not going as you may desire. The more you are open to these types of things the less mental stress you will go through if things don’t go to plan.
– Mother of two with rheumatoid arthritis, Australia (excerpt from
Arthritis, Pregnancy and the Path to Parenthood, by Suzie Edward May
Design Thinking: Or Why Life with RA Forces You to be Creative
Posted by My RAD Life in Dealing, RA/RAD, Symptoms on February 26, 2016
Design Thinking:

Last night I went to a talk on Design Thinking. This is marketing/business jargon for approaching product design from a user’s point of view. The speaker encouraged everyone to go out and talk to their end-users so that they could design with empathy.
As an example, she talked about a new pill bottle that her company helped design. (Not sure what the product is, otherwise I’d post it.)
Her colleague went out and interviewed some older patients in their homes. Noticing an older woman’s severely arthritic hands, he asked her whether she had any trouble taking her medications at home. She replied that she had no problems at all.
He asked her to walk her through her medication routine, so she led him to her kitchen and showed him the electric meat slicer she used to open her pill bottles.
Yes, you read that right. She used this

to open these
But the thing is, from her perspective – her “new normal” – she was doing just fine.
The product designer disagreed and apparently designed pill bottles that were easier to open.
This is a great little anecdote to encourage product designers to actually meet their intended product users, but that’s not really what I got out of it. I found this woman pretty damn inspiring. Here she is, with severe arthritis, and she’s making it work with the tools she has. She’s not whining. From her point of view, she’s just fine.
Design Thinking & RA:
This morning I was woken up by my right wrist, which was so stiff and painful I couldn’t move it. So I drag myself out of bed, take a really long, hot shower, and wait for my wrist to feel a bit better. No luck.
I dig out my wrist brace and attempt to brush my hair/teeth and apply make-up left-handed. Fun!
Then I go to work and try to operate my mouse with my left hand.
Now, I’m not as bad-ass as the woman in the story above. If anyone asked me if I was having trouble today, I’m pretty sure I would be a flood of complaints. But with diseases like RA, you’re forced to roll with the punches and get creative in how to compensate.
I’m happy to say that I went for a jog in the sun this afternoon and though still painful, my wrist is now doing a bit better (I’m typing this after all!).
Design Thinking as applied to life with RA:
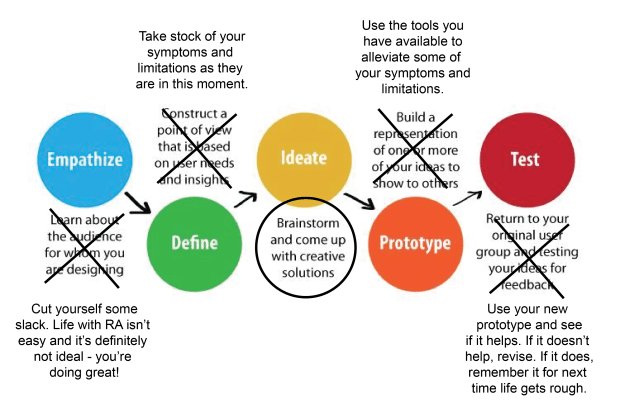
Have You Tried Fish Oil?
Posted by My RAD Life in Alternative Medicine, Dealing, Diet, Drugs, RA/RAD, Symptoms on February 23, 2016
I live in a city that embraces naturopaths, acupuncture and supplements. Anytime I tell anyone I have Rheumatoid Arthritis, they immediately follow with diet or supplement advice.
Fish oil cures that, right? MSM eliminates symptoms. Add turmeric!
This advice is not only coming from the uneducated. I’ve read books and studies recommending some supplements, including fish oil, from reputable sources.
When I was first diagnosed, I heeded this advice. It got to a point where I was taking a handful of pills morning and night.
Finally, my body had enough, which it communicated with a gag reflex I started getting just by seeing the vitamins in my hand. I’m currently listening to my body and taking just one supplement each day – alternating calcium/vitamin D with a hair, skin and nails formula (does wonders for my methotrexate-induced hair loss and weak nails!).
Last night, I finally got around to watching Frontline’s Supplements and Safety documentary.
It’s an important watch for anyone who adds supplements to their daily regimen.
I won’t pretend to be a doctor and offer medical advice. Some people get great results from supplements. Just please add them to your diet with caution and awareness that the industry is not regulated!
